Arthritis is an umbrella term with many divisions and subdivisions. There are many types of arthritis, and unlike what people usually think, it is not only limited to older adults.

As you will see in this article, there is a type of juvenile arthritis and other types that are very common in young people.
Moreover, we will make a brief review of the signs and symptoms of rheumatoid arthritis and evaluate how patients typically experience the disease throughout their lifetime.
Juvenile Arthritis vs. Adult Arthritis
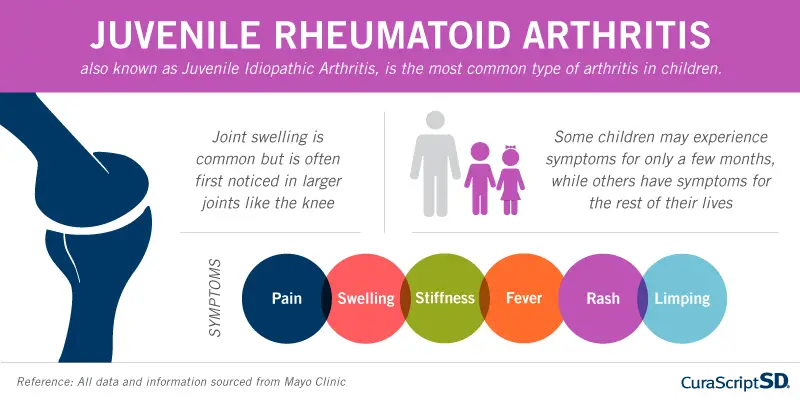
The age of onset of arthritis is highly variable, and there’s a variety called JRA, or juvenile rheumatoid arthritis. It is also known as juvenile idiopathic arthritis because the initial trigger is not yet fully understood. Teenage Juvenile arthritis appears in young children aged 16 years or younger. It is the most common type of arthritis in young children and causes inflammation of the joint and bone growth problems in children and adolescents.
Unlike adult arthritis, the juvenile variant does not always cause significant joint pain. Joint soreness is common, but not a rule to make the diagnosis. Instead, what we always have is a limitation in the mobility of the articulations. These children also display signs of inflammation that include swelling, warmth, and redness of the joint.
Osteoarthritis in Young and Active people
with thanks www.ncbi.nlm.nih.gov
Similar to adult arthritis, this juvenile type is significantly modulated by genetics, but the environmental conditions may contribute to triggering the condition. Besides the compromise in the musculoskeletal system, it causes problems in the heart, eyes, lungs, and nervous system of affected children.
The episodes of JRA can be recurrent, but in the majority of cases, the disease is self-limited, it does not cause a lifelong illness and does not leave any significant disability. However, in some instances, JRA can progress to adult rheumatoid arthritis, especially in young patients who have a positive rheumatoid factor.
What are the expected aches and pains at 40?
Rheumatoid arthritis in adults usually appears somewhere between ages 30 and 50. The age of onset is widely variable, and there is also a late-onset type of rheumatoid arthritis we are covering further. For educational purposes, and to explain the progression of the disease, we are going to give an example of a patient with rheumatoid arthritis who started experiencing symptoms at the age of 40 years old.
In the majority of cases, arthritis in this age starts very insidiously. There’s a slow development of the typical signs and symptoms that include swelling, stiffness, and pain. This insidious onset can be extended over a few weeks or months. The pain and stiffness can be limited to one joint or can be located in multiple joints, which is more common. Most patients will also experience significant tenderness to the touch.
In this early stage, rheumatoid arthritis commonly affects the metacarpophalangeal joint or the interphalangeal joint of the hand. It may also affect the wrist or the metacarpophalangeal joint of the feet. In most cases, musculoskeletal symptoms are accompanied by fatigue and malaise. Patients often feel depressed and reduce their energy levels. Fever is also common, especially during flares, but it is low grade, never higher than 100 °F unless there’s another disease or infection.
In some cases, patients may experience tenderness and swelling in one or two joints for a while. After a few days, the symptoms go away and return in another set of joints with the same intensity. Still, the disease is widely variable, and we can have a patient with a violent onset of explosive polyarticular pain and stiffness that develops in one or two days.
What are the expected aches and pains at 50?
After around 10 years from the first onset of symptoms, and without proper care and medical attention, arthritis is likely to advance to a stage 2 and stage 3, which is considered severe arthritis. In these patients, the damage to the articulation extends beyond the synovium to the cartilage and the bone. As rheumatoid arthritis reaches the cartilage, patients start to experience loss of mobility of the articulation, and their stiffness becomes worse and more limited.
In stage 3, uncontrolled arthritis becomes severe, and the bone ends are almost bare in the articulation, with no cartilage in-between. Thus, they rub together and cause significant pain and inflammation in the articulation. These patients have a significant loss of mobility and may also experience muscle weakness due to erosion and deformity of the bone. The process of deformity has already started, but it is not as severe as in stage 4.
Consider that these aches and pains at the age of 50 are based under the assumption that rheumatoid arthritis has started at the age of 40, and the patient has not completed his medical treatment. In most cases, following medical advice can slow down the progression of the disease and spare patients from the long-term consequences of this disease.
What are the expected aches and pains at 60?
At the age of 60, patients with a 20-year progression of rheumatoid arthritis and without medical treatment may enter a stage 4, which is the most severe, end-stage of rheumatoid arthritis, where the bone ends are entirely eroded, and the articulations stop working. In some cases, the joints are not only destroyed but fused together, and the muscles are completely lost and damaged. These patients typically have significant pain, mobility loss, disability, and impaired quality of life.
The disease is highly variable, and some patients at the age of 60 still have a stage 2 arthritis that allows them to move around and live a relatively normal life. There is also a late-onset rheumatoid arthritis, which has its onset at the age of 60 and older. These patients usually have an acute instead of an insidious onset, and it typically affects large joints (shoulders and knees) instead of small joints (fingers and toes). It is usually less severe unless the rheumatoid factor is positive, which may be the case in aggressive cases of late-onset rheumatoid arthritis.
References:
Oen, K., Malleson, P. N., Cabral, D. A., Rosenberg, A. M., Petty, R. E., & Cheang, M. (2002). Disease course and outcome of juvenile rheumatoid arthritis in a multicenter cohort. The Journal of Rheumatology, 29(9), 1989-1999.
Felson, D. T., Smolen, J. S., Wells, G., Zhang, B., Van Tuyl, L. H., Funovits, J., … & Brooks, P. (2011). American College of Rheumatology/European League Against Rheumatism provisional definition of remission in rheumatoid arthritis for clinical trials. Arthritis & Rheumatism, 63(3), 573-586.
Katz, P. (2017). Fatigue in rheumatoid arthritis. Current rheumatology reports, 19(5), 25.
Villa-Blanco, J. I., & Calvo-Alen, J. (2009). Elderly onset rheumatoid arthritis. Drugs & aging, 26(9), 739-750. Innala, L., Berglin, E., Möller, B., Ljung, L., Smedby, T., Södergren, A., … & Wållberg-Jonsson, S. (2014).
Age at onset determines severity and choice of treatment in early rheumatoid arthritis: a prospective study. Arthritis research & therapy, 16(2), R94.
